We’re very excited to publish a study looking at patients undergoing appendicectomy in GlobalSurg 1.
The use of laparoscopy in low-income settings is controversial, yet many of our collaborators report the apparent benefits and wish they could do more.
The purpose of the study was to compare outcomes in the laparoscopic compared with the open group.
This is always difficult out-with a randomised controlled trial. Hospitals that can do laparoscopy are better resourced thank those that cannot. Moreover, surgical teams with laparoscopic capabilities may choose an open approach for more difficult patients. For instance, those with a perforated appendix and sepsis. So observational data are biased.
To try and overcome that bias, this study uses propensity-score based matching. This utilises all the information we have about patients and hospitals to create laparoscopic and open groups that are balanced. This means that the characteristics of patients in each group should be similar, for example, the same number of perforated appendices, the same number of males/females etc. To an extent, it tries to replicate what happens in a randomised trial for observational data.
Bias (confounding) will still exist for patient characteristics not captured in the study, for example, patients unwell with sepsis.
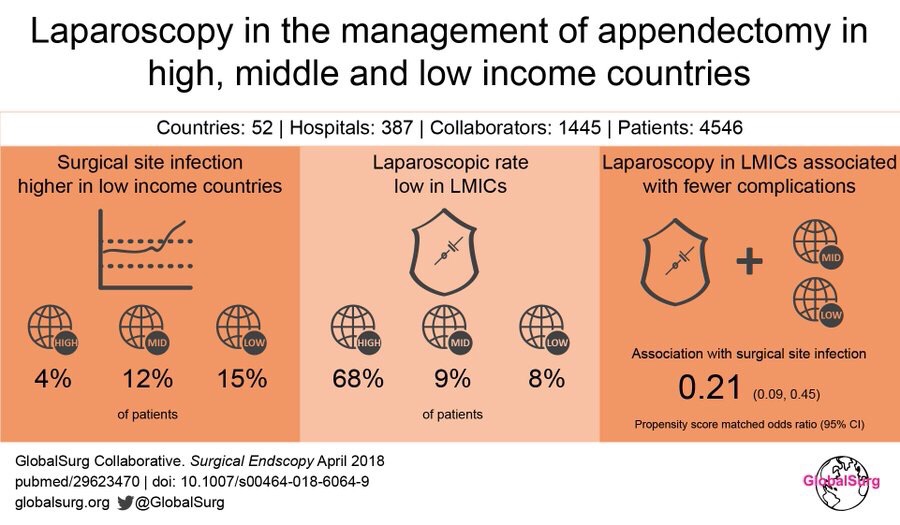
On performing this analysis for patients in low and middle income countries only, a clear benefit of laparoscopy over open surgery is seen. It is possible that the actual benefit is not as large as this given the observational nature of the data.
However, as best as we can see with these data, lap has significant benefits over open.
There are many issues with the introduction of laparoscopy when resources are stretched. We talk about these in the discussion of the paper. We conclude,
There are profound clinical, operational, and financial barriers to the introduction of laparoscopy that if overcome could result in significantly improved outcomes for patients and the wider health system in low-resource environments.

Leave A Comment