Congratulations to Dr Brendan Berry winner of the GlobalSurg Research Prize at the 2017 Association of Surgeons in Training (AsiT) annual meeting held in April in Bournemouth, UK.
In this guest blog Dr Berry describes his awarding project and the experience of conducting his research in South Indian.
Can Three Dimensional (3D) Printing Technology Offer Economic Advantages For Disadvantaged Patients In Resource Poor Countries Who Require Complex Craniofacial Surgery?
Authors: Dr Brendan Berry, Dr Derick Mendonça
Work supported by: Scar Free Foundation, SAKRA World Hospital, Osteo3d
Whilst working in south India for 10 weeks in the field of craniofacial plastic surgery, I saw a huge variety of complex procedures undertaken on patients who often presented late to hospital and with far more disfiguring and complex conditions than one would see in the UK. This was often due to lack of personal finances or hospital facilities close to their homes. Poor social understanding of complex craniofacial pathology in India also means that many of these individuals lead lives of greater isolation in fear of being shunned by their societies.
Myself and supervisor Dr Mendonca along with Osteo3D, a fantastic start-up company in Bangalore, have been keen to find ways to make surgery more affordable and available to those who need it most. This project discusses the latest use of 3D printing technology within plastic and maxillofacial surgery and explains how its use can have significant advantages over more conventional surgical approaches.
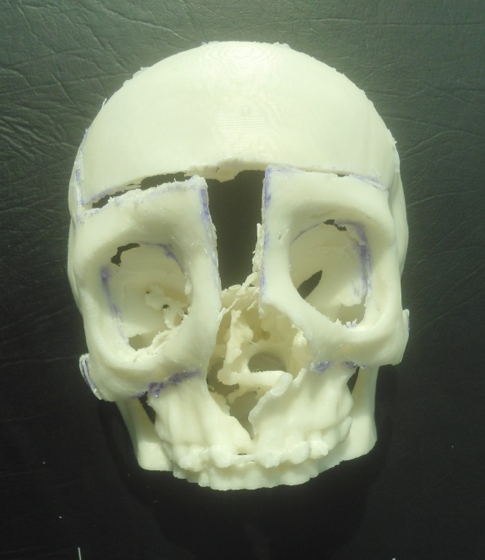
The primary outcome was to identify whether practicing operations on 3D printed models made from a patient’s CT scans, could reduce operating times when it came down to the actual procedure? Secondary outcomes included looking at whether there were reductions in: anaesthetic time, length of hospital stay, the number of revision operations undertaken.
To find this out, retrospective data was collected from patients who underwent complex craniofacial surgery in Bangalore, at 3 hospitals within the last 2 years. To analyse the data, patients who received 3d printing in the planning stages of their operations were matched to patients who did not. To avoid selection bias, the paired patients were randomly linked according to; the operating surgeon, the operation type and the year the operation was undertaken.
The results of the study highlighted a significant reduction in operating time amongst those receiving 3D printing in the planning stages of their operations. On average a mean time reduction of 21.7% was observed, which correlates to a 77-minute reduction per operation. Reductions in anaesthetic time of 11.1% were also observed. No significant difference in length of hospital stay or number of revision operations was observed between the two groups.
In conclusion, this study has shown that by using 3D printing in the planning stages of complex craniofacial surgery in lower income countries, reductions in operating times by almost a quarter can be observed. It has also shown that by reducing operating times, huge financial benefits to both the patient and healthcare provider can occur.
Most importantly, health benefits can also be gained by using 3D printing in this way, including reductions in anaesthetic risks and potentially operative blood loss. With than 10% of complex craniofacial cases utilising the benefits of 3D printing in the planning stages of such operations, greater attention is needed to make other surgeons and patients aware of these benefits.







Leave A Comment